Diabetic retinopathy develops when prolonged high blood sugar damages retinal blood vessels, leading to leakage, ischemia, or abnormal vessel growth. Early stages may not affect vision, but progression to macular edema or proliferative disease significantly increases the risk of permanent vision loss.
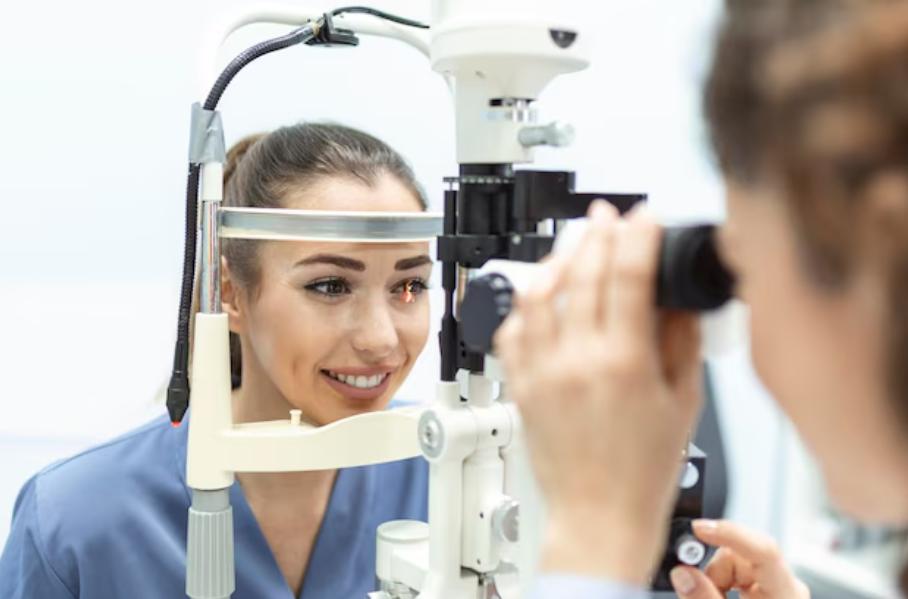
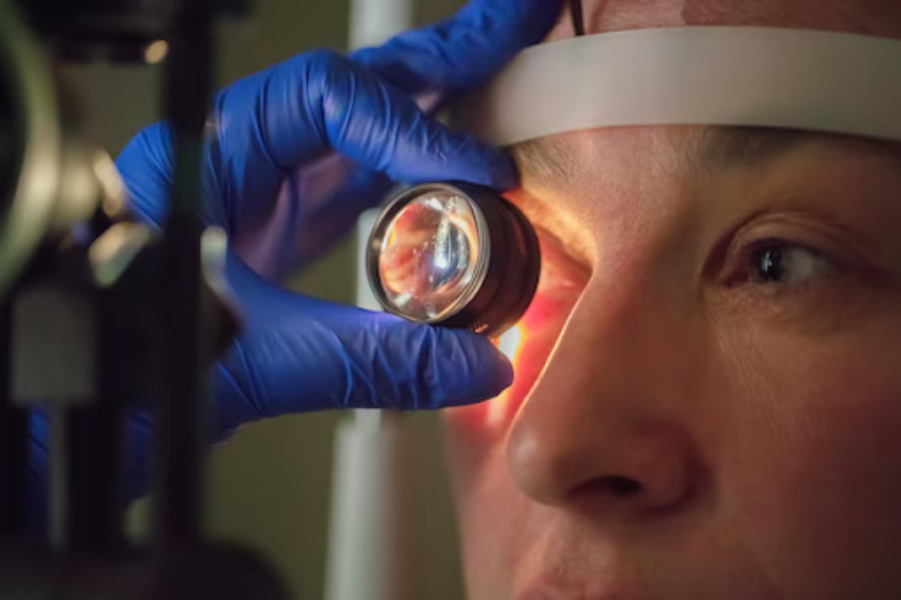
At Dr. Jyotis Hospital in Panchkula, retinal evaluation begins with OCT imaging to measure macular thickness and detect fluid accumulation. This allows differentiation between non-proliferative diabetic retinopathy, where monitoring may be sufficient, and sight-threatening disease that requires active treatment.
Intravitreal injections are used when macular edema or neovascular activity is present. These injections target vascular growth factors responsible for leakage and swelling. Treatment intervals are adjusted based on anatomical response seen on repeat imaging rather than a fixed injection schedule.
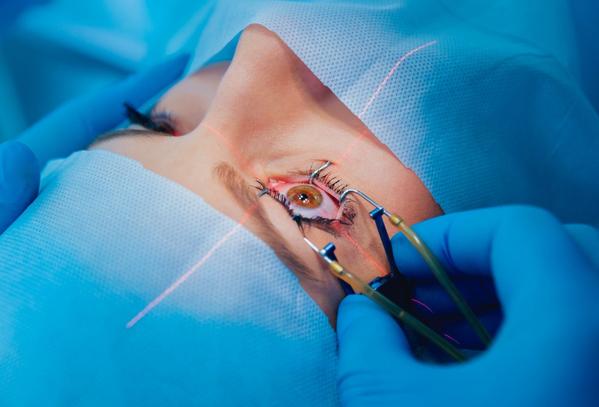
Laser photocoagulation is reserved for specific indications, such as proliferative diabetic retinopathy or areas of retinal ischemia. Unlike injections, laser treatment aims to stabilise the retina and reduce the risk of vitreous hemorrhage rather than improve immediate visual acuity.
If diabetes-related vision changes or OCT abnormalities have been identified, targeted retinal treatment can help preserve central vision and reduce long-term complications.