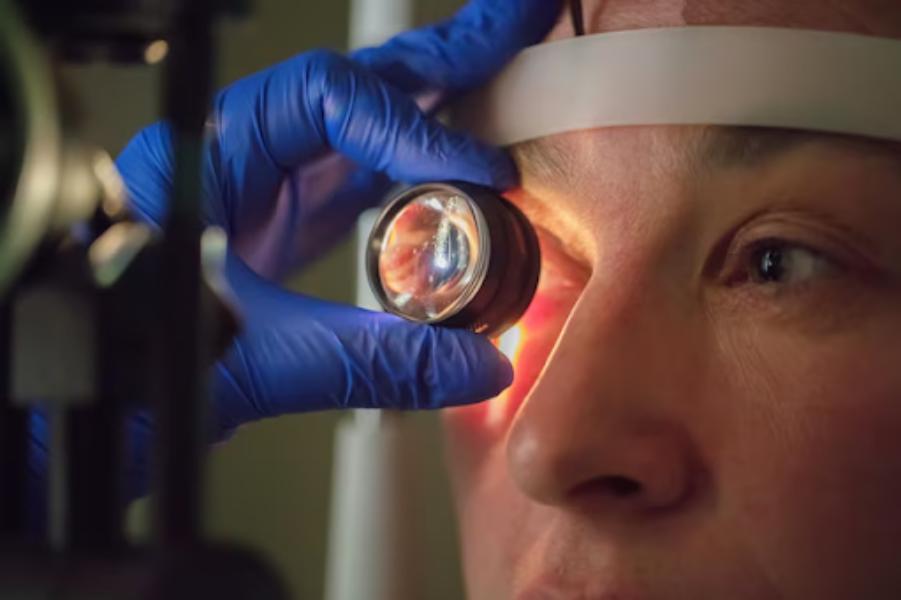
Eye surgery is rarely a single-category decision. Patients may require surgical correction for cataracts, glaucoma, corneal disease, retinal complications, or trauma-related structural damage. Each condition demands a different surgical pathway, and outcomes depend heavily on identifying the exact structure responsible for vision loss.
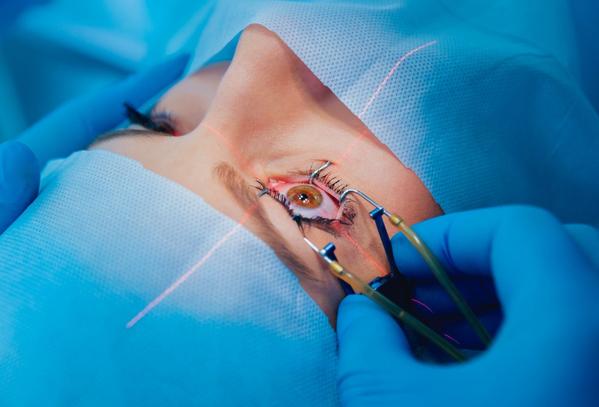
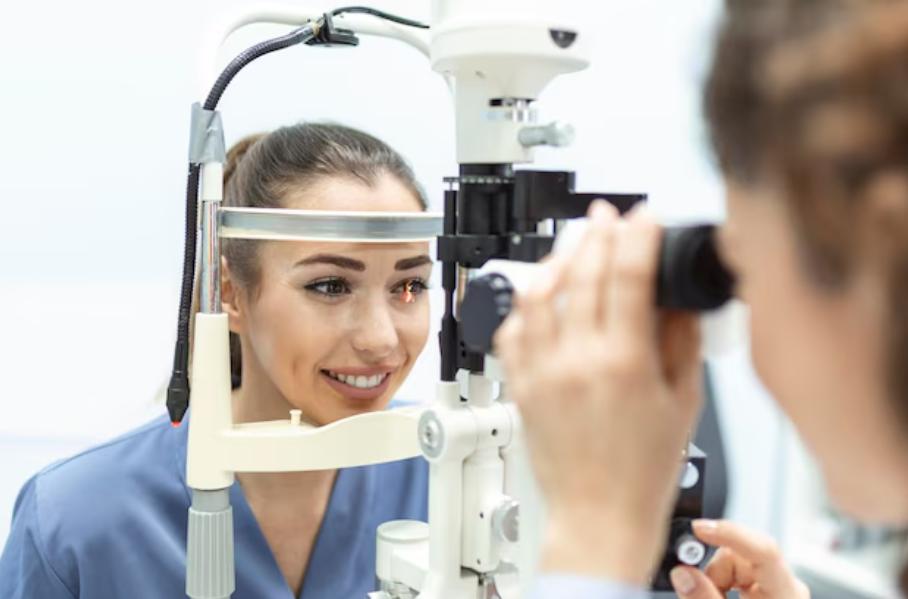
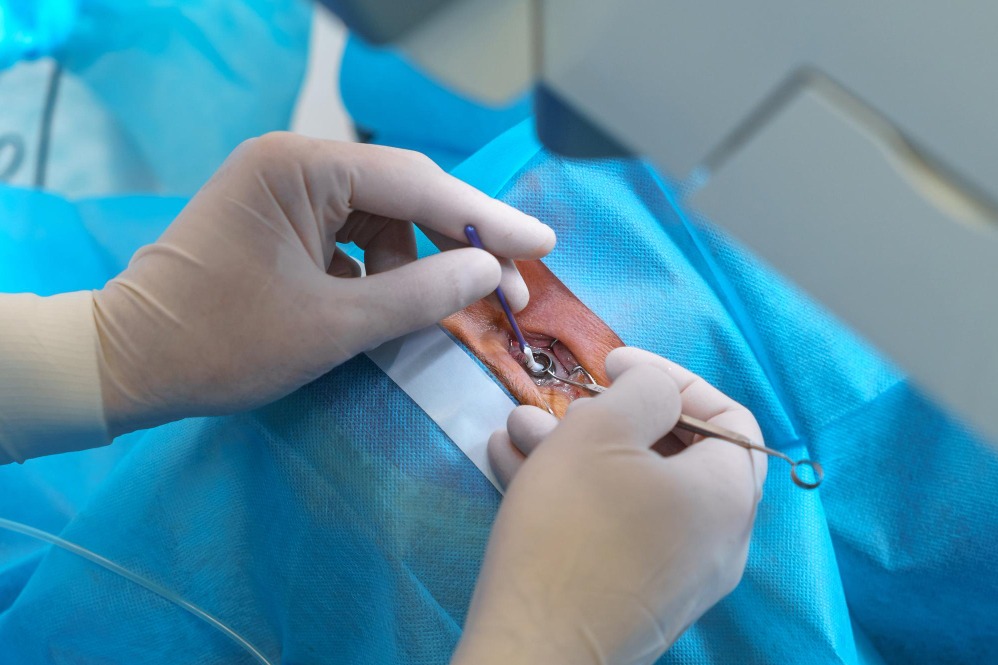
At Dr. Jyotis Hospital in Mohali, surgical evaluation begins by separating reversible vision loss from progressive disease. Cataract surgery addresses lens opacity, while glaucoma surgery focuses on improving aqueous outflow to reduce optic nerve damage. Retinal surgeries, such as vitrectomy, are considered only when internal eye bleeding, traction, or detachment threatens vision stability.
Surgical planning takes into account corneal thickness, pupil dilation, retinal status, and systemic conditions like diabetes. These factors influence not only the type of surgery but also anesthesia choice, incision technique, and recovery expectations. Patients with coexisting eye diseases often require staged or combined procedures rather than a single operation.
Risk assessment is a critical step. For example, glaucoma surgery carries pressure-related risks, while retinal surgery involves positioning and prolonged recovery considerations. Addressing these factors before surgery helps align expectations with realistic outcomes.
If surgery has been advised or vision continues to decline despite medical treatment, a condition-specific surgical consultation can help clarify whether intervention is necessary and which approach is most appropriate.