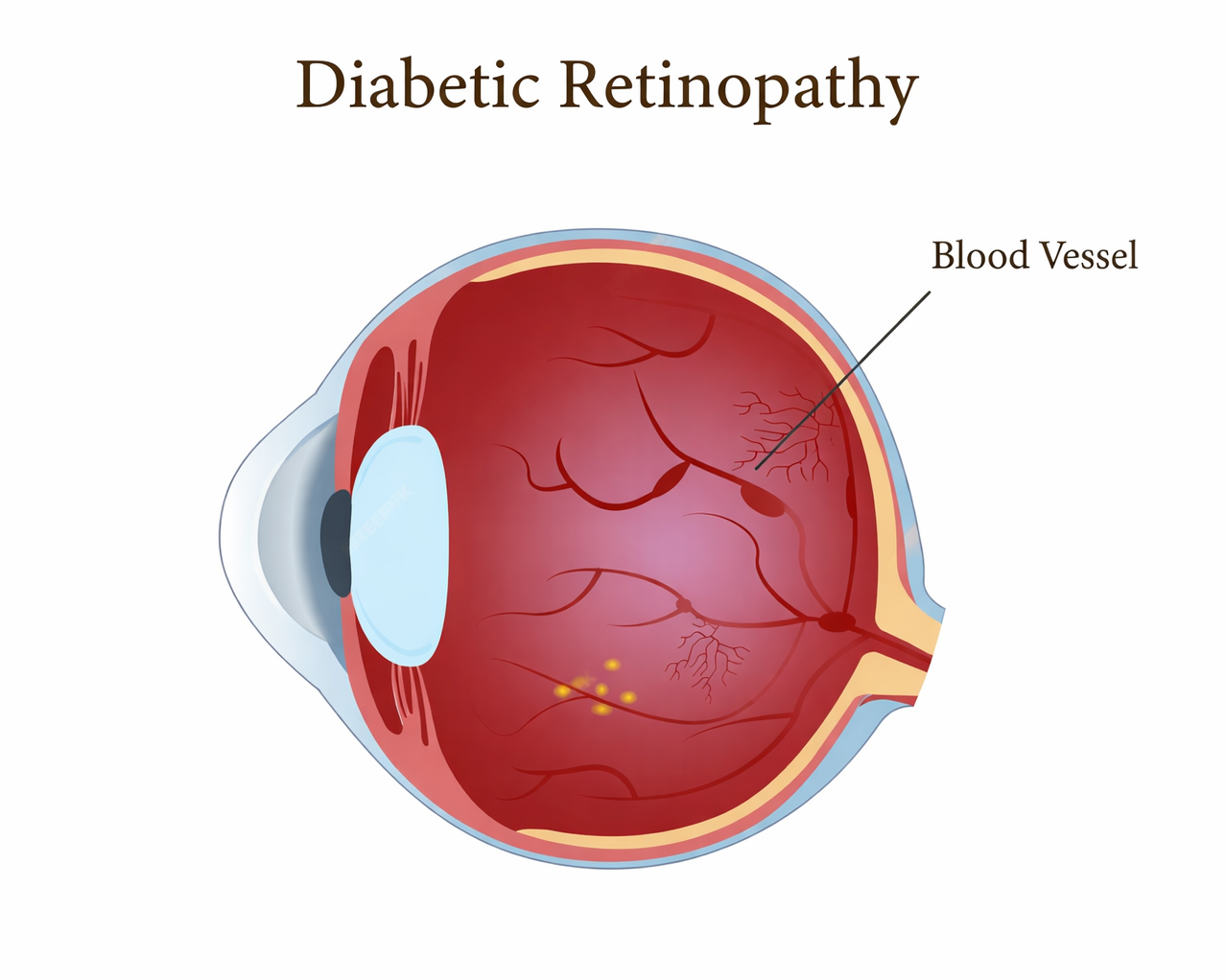
Diabetic retinopathy develops when prolonged elevated blood sugar damages retinal blood vessels, leading to leakage, ischemia, or abnormal vessel growth. Early stages often progress without visual symptoms, making structured evaluation important for timely intervention.
At Dr. Jyotis Hospital in Panchkula, diabetic retinopathy assessment focuses on defining disease stage rather than relying solely on visual complaints. Non-proliferative changes may only require observation, while macular edema or proliferative disease demands active treatment to reduce the risk of permanent vision loss.
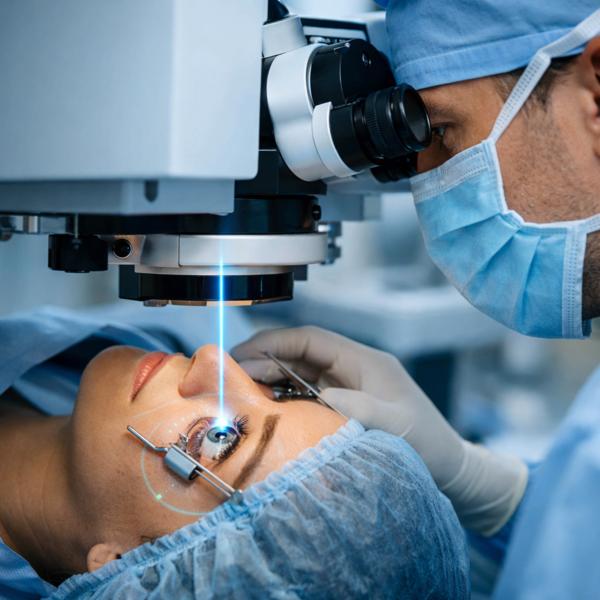
Treatment selection is stage-specific. Macular edema is commonly managed with intravitreal injections to control swelling, whereas proliferative diabetic retinopathy may require laser photocoagulation to reduce abnormal vessel growth. Advanced cases complicated by vitreous hemorrhage or traction may need surgical intervention.
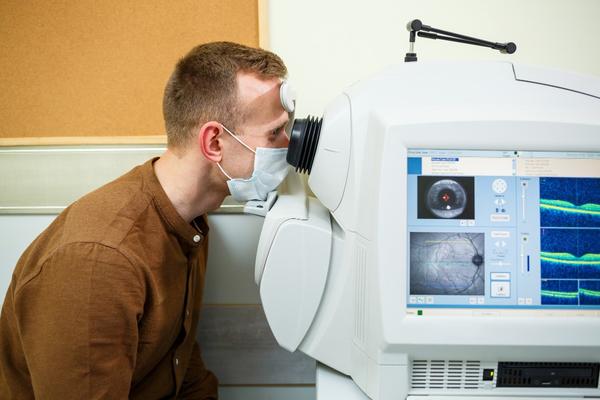
Imaging findings guide decisions more reliably than symptoms. Structural worsening often precedes noticeable vision decline, making OCT and retinal examination central to disease management.
If diabetic retinal changes have been identified, stage-appropriate treatment can help slow progression and protect remaining vision.